Population Health, Based Upon the Asheville Project
Interactive platform allowing clinical care managers to access population health data, record notes, bill visits and more
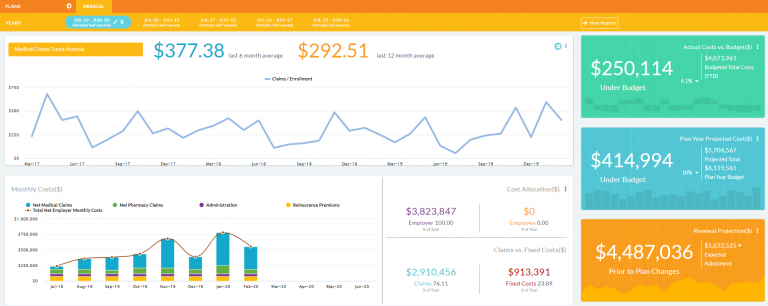
Interactive platform allowing clinical care managers to access population health data, record notes, bill visits and more
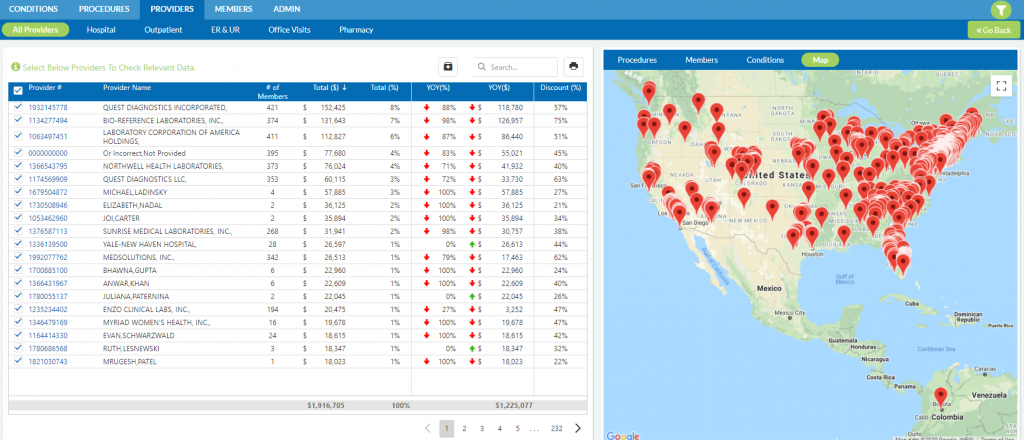
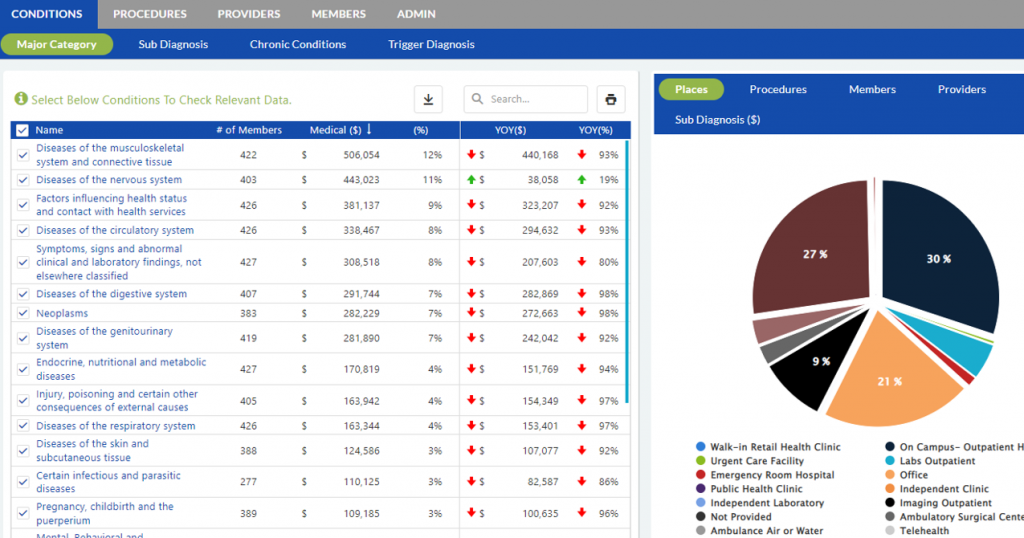
Multiple dashboards and functionality to search large claimants or drugs on an individual client or block of business level.
When a member has a claim, there obviously is always a condition, procedure and provider attached to that claim. For that intuitive reason, our search functionality always keeps these items linked when searching various items on the entire population. By linking these our clients find that navigating their data becomes ore simple than ever.
We also provide firm level dashboards to roll-up the results on your entire block of business.

Measure the effectiveness of your disease management programs with condition level risk scoring on a population or member level.
Claim analytics provides self-insured employers with the ability to easily unlock the claims data on their healthplan. Our platform consolidates your medical, pharmacy, clinical, and biometric data from your TPA and PBM. We then scrub, normalize, and quality check the data before loading it to your white-labeled portal.